Eczema is a common inflammatory skin condition that affects people of all ages and it can cause discomfort and pain. In fact, this condition is so common that 1 in 5 children and 1 in 10 adults in Ireland are affected by it. But what is it? What causes it? What treatment options are available? Let’s take a closer look!
What is Eczema?
As mentioned, Eczema is a chronic inflammatory skin condition. It causes the skin to become inflamed, dry, irritated and itchy. You might be thinking “this sounds like dermatitis”, and you would be right. Dermatitis is a general term used for conditions that cause inflammation of the skin. Atopic dermatitis is the medical term for eczema. For most people, eczema symptoms will follow a relapsing and remitting pattern over the course of weeks or months. When symptoms worsen, it is known as a flare-up. Unfortunately, there is no cure for eczema but there are ways that you can reduce the severity and frequency of flare-ups, but we’ll come back to that a little later on.
What Causes It?
The exact cause of eczema is unknown, it is felt to be multifactorial; autoimmune (inappropriate activation of the immune system), stress, genetic factors and environmental triggers. These factors cause changes in the skin barrier that impair its protective function. Essentially, the skin acts as a barrier to help protect us against irritants, allergens, chemicals, UV light, infection, and water loss.
Eczema typically develops in childhood and certain factors are thought to be important in this development. For instance, genes could play an important role; it is possible that one could have a genetic predisposition to having a weakened skin barrier. Similarly, altered inflammatory and allergy responses could play a significant role.
What Are The Most Common Symptoms?
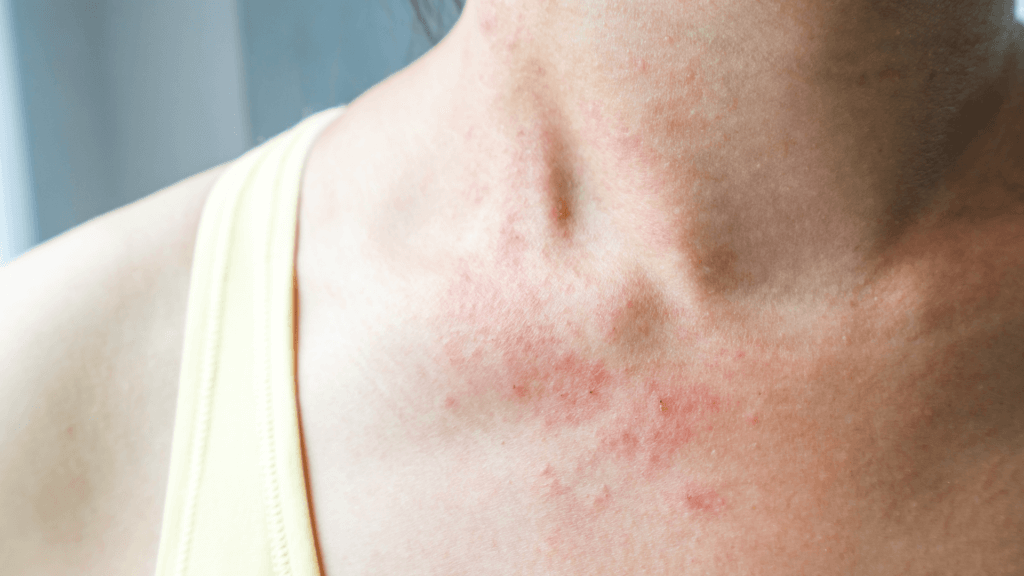
Eczema is most commonly characterised as dry, red patches appearing on the skin. These patches can be extremely itchy and the skin can become quite dry and flaky. Eczema can occur in many different parts of the body, but it most commonly appears on the face, arms, elbow creases, hands, and the backs of the knees.
There are different types of eczema and the pattern and severity of symptoms can differ from person to person. For instance, some people may experience dry, flaky skin, but others may experience blistering of the skin. The itching sensation associated with eczema can be very intense, often disturbing sleep. However, it is important not to scratch eczema as scratching can damage the skin, leaving open sores which are prone to infection and scarring. If present for a long time, eczema can also cause the skin to become thick and hard. Let’s take a closer look at the different types of eczema and the symptoms associated with each.
What Are The Different Types of Eczema?
There are seven different types of eczema, each with its own characteristics and symptoms.
Atopic Eczema
Atopic eczema, also known as atopic dermatitis, is the most common form of eczema. It usually develops in childhood and gets milder over time. Atopic dermatitis can run in families and it frequently occurs alongside other atopic conditions, such as hay fever and asthma.
Atopic dermatitis appears as patches of red, dry skin, often forming in the creases of the elbows or knees, but it can appear anywhere on the body. Babies and small children will often get this rash on their cheeks and scalp. You may also notice small bumps forming which will leak fluid if you scratch them. We strongly recommend refraining from scratching as the skin can become infected. This also allows the scratch-itch cycle to continue which can make the intensity of the itch worse.
Contact Dermatitis
Contact dermatitis looks very similar to atopic dermatitis as it will appear as patches of red, irritated skin. However, contact dermatitis is caused by exposure to certain substances. There are two different types:
Allergic contact dermatitis: is caused by an immune system reaction to an irritant, such as latex or metal.
Irritant contact dermatitis: is caused by exposure to a chemical or other substance that irritates your skin.
In addition to red, itchy skin, contact dermatitis can cause hives to appear on the skin. Fluid-filled blisters may also form. Here are some of the most common triggers for contact dermatitis:
- Laundry detergents
- Soaps, shampoos, bubble baths
- Perfumes and make-up products
- Solvents
- Tobacco smoke
- Cleaning products, such as bleach
- Paint
- Nickel
- Latex
- Jewellery
Dyshidrotic Eczema
This form of eczema most commonly affects the hands and the feet. It causes fluid-filled blisters to form on the toes, soles of the feet, palms, and fingers. These blisters can become sore and itchy. In addition, the skin can crack and become flaky or scaly. The exact cause of this type of eczema is not known, but it is more common in those who have another type of eczema and it tends to run in families. Some of the most common triggers for Dyshidrotic eczema include:
- Damp hands and feet
- Stress
- Smoking tobacco
- Allergies
- Exposure to substances, such as cobalt and nickel
Neurodermatitis
This form of eczema is very similar to atopic dermatitis as it causes scaly patches to appear on the skin. However, this form tends to be widespread across the body, whereas atopic dermatitis is limited to patches of the skin. This form of eczema is more likely to affect those who have other types of eczema or psoriasis and stress is a known trigger.
Nummular Eczema
Nummular eczema is very easy to recognise as it causes round, coin-shaped spots to form. This form is extremely itchy and is often triggered by a reaction to chemicals or insect bites. Dry skin is also a known trigger. Like neurodermatitis, nummular eczema is more likely to affect you if you have another type of eczema.
Stasis Eczema
Varicose eczema is caused by fluid build-up in the lower limbs as a result of varicose veins, circulation problems or heart disease. It leads to discolouration of the skin, dry thickened skin and often intense itching. In some cases, it can be associated with skin ulcers.
Ways to Limit Flare-Ups
The most important thing you can do to reduce the frequency and severity of flare-ups is to support the protective barrier function of the skin. To do this, you will need to make sure the skin stays hydrated. To do this, you can:
- Use emollients (moisturisers), such as creams, ointments and soap substitutes to help restore moisture levels in the skin.
- Moisturise as part of your morning and nighttime skincare routines.
- Consider adding hyaluronic acid (HA) to your skincare routine between flare-ups – this will gently draw moisture into the skin.
- Make sure you drink plenty of water.
- Avoid harsh or alcohol-based cleansers which will dry out the skin.
- Avoid scrubs, hard facecloths, and face wipes as they dry out the skin.
There are many moisturisers to choose from – the best one is the one that you like. Regardless of what treatment you are using, it is essential that you keep your skin well moisturised by using liberal amounts of moisturiser regularly (3-4 times daily), even when your skin is in good condition. This is the most important part of eczema management.
CAUTION: When moisturisers dry on dressings, clothing, bed linen or hair they can catch fire very easily if they come into contact with a naked flame. It is essential that extra care is taken around naked flames (e.g. candles, cigarettes) when using skincare or hair care products. It is advisable to wash clothing and bed linen regularly if it has been in contact with moisturisers. Please note the moisturisers are not fire hazards when in their containers – it is only when they have dried out on these materials.
Know What Triggers Your Eczema
As we know, there are many different factors that can trigger a flare-up of symptoms. If you know what triggers your eczema symptoms, limit exposure or avoid them where possible. Here are some examples of the most common triggers for eczema:
- Irritants: shampoos, bubble baths, soaps, detergents, fragrances, materials such as wool, changes in temperature
- Stress
- Infection or illness
- Allergens: dust mites, pollen, animal dander
Be Gentle With Your Skin
Try to be gentle with your skin, even between flare-ups. Using skincare and make-up products that are specifically formulated for sensitive skin will help prevent irritation. Similarly, you should avoid tight-fitting clothing, heavily fragranced cosmetics and laundry detergents.
As mentioned above, changes in temperature can trigger symptom flare-ups. Whilst it might be difficult with Ireland’s ever-changing weather, we recommend changing your skincare routine as the weather changes. Colder weather dries out the skin, as does central heating when you’re spending more time indoors. Therefore, we recommend opting for a heavier moisturiser in the winter months. Sun exposure may also trigger symptoms, so you should limit time spent in direct sunlight and always wear SPF.
If you’re trying out new skincare or make-up products, we recommend doing a patch test beforehand. This means applying a small amount of the new product to a small area of the skin where the product will be used. Monitor this area for 24 hours and assess for any reaction before you use the product anywhere else. This will give you a chance to monitor how your skin reacts to the new product. Similarly, we suggest adding products one at a time, over the course of a few weeks. If you start using five different products at the same time, and you have a reaction, it will be very difficult to tell which product caused it!
What Treatment Options Are Available?
Calming inflammation is an important part of treating eczema and while cooling moisturisers and ointments may help, occasionally you may need to use topical steroids. Luckily, topical ointments and creams are widely available. In fact, you can request a prescription for eczema treatment through our online prescription service for mild to moderate eczema.
Webdoctor.ie currently provide prescriptions for:
- Topical steroids (creams & ointments)
- Oral antihistamines
Please note that we can only provide prescriptions for medications listed in our medical questionnaire.
How to Request Eczema Treatment
Requesting a prescription for eczema treatment couldn’t be easier with Webdoctor.ie! Simply fill in a brief medical questionnaire. Once your request has been approved by one of our Irish Medical Council registered doctors, we will send your prescription to an Irish pharmacy of your choice, via secure Healthmail.
Have questions about eczema treatment? No problem, our GPs are happy to answer any questions that you may have. Simply book an online video consultation and we can talk you through the treatment options.
To stay up to date on your treatments and services, join our online communities on Facebook, Instagram and Twitter. There, you’ll also find lots of medically-reviewed insights on skincare, along with other health and wellness topics.







